UTI Evaluation

Indications for imaging in patient with UTI, from Campbell's

Causes for bacterial persistence in UTIs, from Campbell's
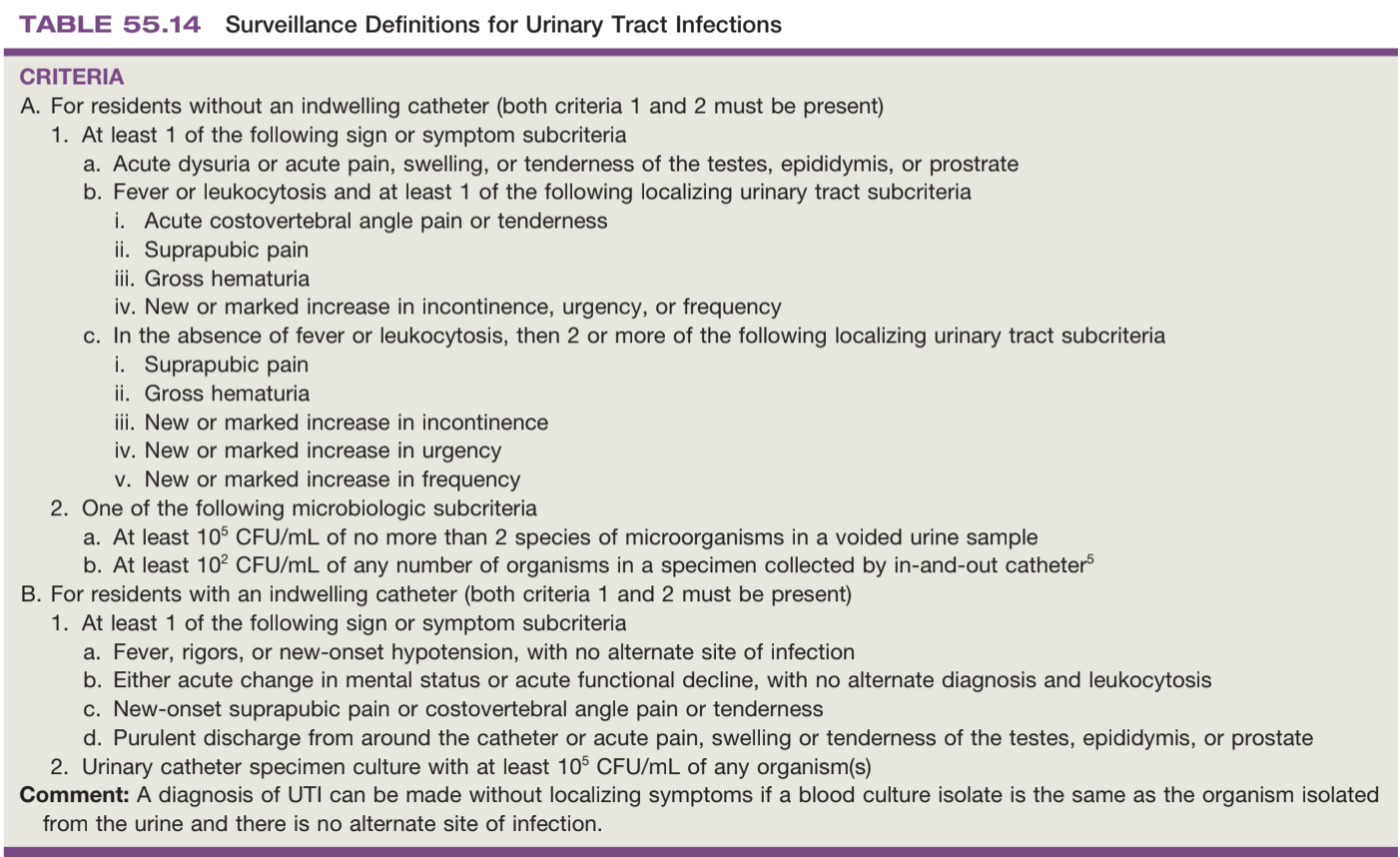
UTI surveillance in high risk patients, from Campbell's
UTI Evaluation
Presenting symptoms
- Common: frequency, urgency, dysuria, suprapubic pain, fever
- Hematuria: can occur with UTI, check UA
- Pneumaturia/fecaluria: high suspicion for fistula
- Differential: pelvic floor dysfunction, STI, reflux, vaginitis/urethritis
Collecting a good urine sample
- Obtain clean catch (0 squamous cells is best sample)
- If tube (foley/PCN) present, consider exchanging tube (if possible) prior to collecting sample
- If ostomy, catheterize stoma for collection
- Do not collect from foley/PCN bag!
Lab Findings
- Leukocyte esterase: sensitive but not specific for UTI
- Nitrites: produced by Enterobacteriaceae, also seen with pyridium
- Cloudy urine: pyuria or precipitated phosphate crystals in alkaline/concentrated urine
- Microscopic UA: presence of bacteruria most indicative
- Mycoplasma/Ureaplasma: appear to be colonizers, unrelated to UTI symptoms, testing not beneficial (per Souders et al JU 2021)
Confounding factors
Asymptomatic Bacteruria
- Definition: bacteria in urine in the absence of any symptoms
- Prevalence: 1-5% healthy young women, 20% women older than 80
- Catheters: 23-89% patients using CIC vs 100% patients with longterm catheter usage
- Screen/treat if: pregnant (increased risk for complications) or undergoing GU instrumentation (increased risk for bacteruria/sepsis)
- Do not screen/treat even if: diabetic, SCI, foreign body in GU tract, prior to non-urologic surgery - no overall benefit and increases risk for resistant organisms
Spinal Cord Injury Patients
- Common UTI symptoms: usually do not have classic symptoms, may show fatigue, fever, vague abdominal/back pain, spasticity, autonomic dysreflexia, new/worsening incontinence
- Recurrent infections: evaluate with upper tract imaging (assess for stones) and urodynamics (high-risk bladder)
- Do not screen or treat asymptomatic bacteruria in patients with SCI and indwelling catheters
- Antibiotic prophylaxis and irrigation have not been shown to decrease bacteruria
- Consider treatment when urease organisms present, may increase risk for bladder stones and catheter encrustation)
References
- AUA Core Curriculum
- Cooper, K. L., G. M. Badalato, and M. P. Rutman. "Infections of the urinary tract." Campbell-Walsh-Wein Urology. 12th ed. Elsevier (2020): 1129-1201.
- Koch, George E., and Niels V. Johnsen. "The Diagnosis and Management of Life-Threatening Urologic Infections." Urology (2021).
- Souders, Colby P., et al. "Mycoplasma and Ureaplasma molecular testing does not correlate with irritative or painful lower urinary tract symptoms." The Journal of Urology 206.2 (2021): 390-398.
- Wieder JA: Pocket Guide to Urology. Sixth Edition. J.Wieder Medical: Oakland, CA, 2021.